Caregivers SPEAK OUT! . . . Norma Myers ~ Author, Advocate, & Mom
Caregivers SPEAK OUT! Norma Myers ~ Author, Advocate, & Mom
presented by
Donna O’Donnell Figurski

1. What is your name? (last name optional)
Norma Myers
2. Where do you live? (city and/or state and/or country) Email? (optional)
Salem, Virginia, USA
3. What is the brain-injury survivor’s relationship to you? How old was the survivor when he/she had the brain injury? What caused your survivor’s brain injury?
Steven was 22 years old. He was involved in a car crash with his brother Aaron. Aaron didn’t survive the accident. Aaron was 26 years old
4. On what date did you begin care for your brain-injury survivor?
August 13, 2012
Were you the main caregiver?
I resigned from my career with Advance Auto and went to Shepherd Center in Atlanta, Georgia, with Steven, but I had complete support from my husband, Carlan. He drove back and forth from Salem to Atlanta to provide support.
Are you now?
Steven lives independently.
How old were you when you began care?
47 years old
5. Were you caring for anyone else at that time (e.g., children, parents, etc.)?
No
6. Were you employed at the time of your survivor’s brain injury? If so, were you able to continue working?
I was employed, but we choose for me to resign so that I could be Steven’s primary caregiver. I returned to the workforce 2.5 years ago – big accomplishment!

7. Did you have any help? If so, what kind and for how long?
I had my husband’s support. We also had offers of help from family and friends. We also received financial support from family and friends through fundraisers.
8. When did your support of the survivor begin (e.g., immediately – in the hospital; when the survivor returned home; etc.)?
Steven was at Carilion Roanoke Memorial Hospital for a month before being transported to Shepherd Center in Atlanta, Georgia.
9. Was your survivor in a coma? If so, what did you do during that time?
Steven was in a medically induced coma. He had a craniectomy (actually, the first of two). (A craniectomy is the surgical removal of a portion of the skull.) We sat by his bedside, and we also planned a life-celebration for his brother Aaron.
10. Did your survivor have rehab? If so, what kind of rehab (i.e., inpatient and/or outpatient and occupational, physical, speech, and/or other)? How long was the rehab? Where were you when your survivor was getting therapy?
Steven received every discipline of therapy available at the Shepherd Center and when he returned home to Virginia. We spent two months at the Shepherd Center for Rehab –

one month, inpatient; second month, outpatient. I spent time learning everything possible about Steven’s rehab needs for when we returned home.
11. What problems or disabilities of your brain-injury survivor required your care, if any?
Getting Steven to his appointments. Making sure we stayed on top of every available resource, including grants, gifts, and programs that would help Steven with his recovery.
12. How has your life changed since you became a caregiver? Is it better? Is it worse?
That is a loaded question. It has changed in many ways, such as I feel like I was there for Steven when he needed me, which I am thankful I was able to do so. We have experienced “firsts” all over again, such as waiting for Steven to speak his first word, to take his first step, and to become independent all over again. It has made me a stronger person because not only have I experienced the death of my first-born son, but I have also experienced what it’s like to watch my other son learn how to do life all over again. 

13. What do you miss the most from pre-brain-injury life?
Witnessing my sons’ enjoying being brothers. I miss being a mother to both of my sons. I also think about what Aaron’s life would look like at every stage of his life if he had survived and what Steven’s life would look like without a traumatic brain injury (Ambiguous Loss).
14. What do you enjoy most in post-brain-injury life?
Celebrating Steven’s victories in life. Helping other families navigate through their journey of TBI (traumatic brain injury).
15. What do you like least about brain injury?
There is no cure, and it’s an invisible disease. I also wish that when people are curious about what happened to Steven, they would ask instead of stare … Steven is fully comfortable in discussing his accident.
16. Has anything helped you to accept your survivor’s brain injury?

Steven’s motto helps me put things into perspective … ”Deficits do not define him.” He is an overcomer.
17. Has your survivor’s injury affected your home life and relationships and, if so, how?
We rearrange life to be available to Steven should he need us if he has a seizure. Currently, with no license due to seizures, we make sure he is where he needs to be all while balancing our careers. We make it work as a family!
18. Has your social life been altered or changed and, if so, how?
Of course! As parents, we will always put our son’s needs first.
19. What are your plans? What do you expect/hope to be doing ten years from now?
I have no idea! We can only take one day – actually one minute – at a time, always trying to better ourselves and be thankful that, while this journey isn’t what we planned for our lives, it’s what God gave us. And we will do the very best we can day by day to honor Him.
20. What advice would you offer other caregivers of brain-injury survivors? Do you have any other comments that you would like to add?

Every brain injury is different, so please don’t do the comparison game. Take one day at a time. Tap into every resource available to you, and, trust me, there are so many out there. You are not alone – there is no shame in asking for help! I will do anything for my fellow brain injury survivors and their families. I am here to offer a word of encouragement through my blogs and volunteer work. Don’t give up!
Get Your Copy Now!
Read It! Listen to It! Review It!

Click Links under Book
AUDIO BOOK Listen to it Now!
Stay Safe and Healthy!
Clip Art compliments of Bing.)
(Photos compliments of contributor.)
As I say after each post:
Please leave a comment by clicking the blue words “Leave a Comment” below this post.

Feel free to follow my blog. Click on “Follow” on the upper right sidebar.
If you like my blog, share it intact with your friends. It’s easy! Click the “Share” buttons below.
 What is your name? (last name optional)
What is your name? (last name optional)

 When Jordan first came home from rehab, she required help with most of her ADLs (Activities of Daily Living). As time has gone on, she has been able to perform most of her ADLs on her own. She has short-term memory loss, so my role is helping to make sure that she remembers things and stays safe.
When Jordan first came home from rehab, she required help with most of her ADLs (Activities of Daily Living). As time has gone on, she has been able to perform most of her ADLs on her own. She has short-term memory loss, so my role is helping to make sure that she remembers things and stays safe.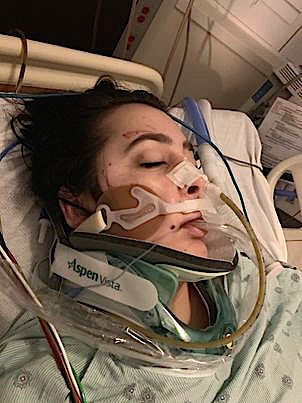


















 13. What do you miss the most from pre-brain-injury life?
13. What do you miss the most from pre-brain-injury life?



 survivor returned home; etc.)?
survivor returned home; etc.)?




 16. Has anything helped you to accept your survivor’s brain injury?
16. Has anything helped you to accept your survivor’s brain injury?



 8. When did your support of the survivor begin (e.g., immediately – in the hospital; when the survivor returned home; etc.)?
8. When did your support of the survivor begin (e.g., immediately – in the hospital; when the survivor returned home; etc.)?
 Take care of yourself.
Take care of yourself. 1. What is your name? (last name optional)
1. What is your name? (last name optional)



 19. What are your plans? What do you expect/hope to be doing ten years from now?
19. What are your plans? What do you expect/hope to be doing ten years from now?

Recent Comments