Survivors SPEAK OUT! Casey Chaffey
Living and Dealing with Chronic Pain
by
Donna O’Donnell Figurski

1. What is your name? (last name optional)
Casey Chaffey
2. Where do you live? (city and/or state and/or country) Email (optional)
Kentucky, USA iluvtkj@yahoo.com
3. On what date did you have your brain injury? At what age?
In 1998, at the age of 22, migraines had become a part of my life.
4. How did your brain injury occur?
Besides the severe head-throbbing, the migraines were often accompanied by nausea, vomiting, extreme sensitivity to light and sound, mental confusion, and more. I gave up caffeine (including chocolate), dairy, and gluten to try to reduce as much inflammation as possible. After being passed from doctor to doctor, I was diagnosed with a vestibular imbalance. That did not improve, even with almost a year of physical therapy, and it became the scapegoat for all of my symptoms.
A few years later, the pain changed from an unwelcome visitor to a permanent resident. Even on my migraine-free days, I still had a persistent headache. Dizziness, blurred vision, fatigue, and constant light-sensitivity decided to join the party as well. Fifteen years after my migraines first started, I was spending about five days a week in bed, and prescription medication was required for me to complete simple daily activities. Finally, after trying more than eighteen different prescriptions and seeing ten different doctors, I had a diagnosis. A fairly large cyst had been growing in the middle of my brain and putting pressure on my optic nerve, which is what caused the vision issues.
When I was 38 years old, a neurosurgeon removed the cyst. Recovery was not easy or quick. I had double vision for more than four weeks. My brain felt exhausted all the time, and I could not look at any screens (TV, phone, or computer). I had a panic attack for the first time in my life. I had to rest a lot. And my hypothalamus was damaged.
However, the moment I woke up from surgery, my constant headache was gone. I no longer felt and heard my pulse in my head. I went from migraines five days a week to six or seven days a month. My dizzy spells rarely show their unwelcome face anymore. I still have limitations and light-sensitivity, and I am always in some level of pain. My blurry vision will occasionally return, and an MRI (magnetic resonance imaging) in 2019 showed evidence of a small stroke at some point. In spite of that, I am thankful for how far I’ve come.
5. When did you (or someone) first realize you had a problem?
See above.
6. What kind of emergency treatment, if any, did you have?
I’ve had treatments, but I didn’t go to the Emergency Room of a hospital.
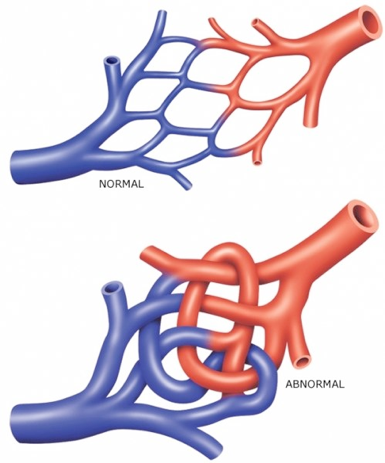
There are two types of brain injury. Traumatic brain injury is caused by an external force, like a blow to the head or an object passing through the skull. A non-traumatic brain injury is caused by internal factors, such as a lack of oxygen or pressure from a tumor. I had both a cyst that put pressure on my brain for many years (non-traumatic). Surgical tools that were used to get to the center of my brain to remove the cyst (traumatic).
7. Were you in a coma? If so, how long?
No
8. Did you do rehab? What kind of rehab (i.e., inpatient or outpatient and occupational and/or physical and/or speech and/or other)? How long were you in rehab?
I did not do any clinical rehab. My husband helped me go for walks, even when I didn’t want to. We started by just going to the end of our short driveway and back. We slowly worked our way up to crossing the street and then circling our small cul-de-sac. When we decided to attempt a loop at the park, I eventually made it. As I continued to push through, the distances grew.
When I was one day shy of being three-months post-op, I stood at the starting line of a half marathon in Nashville, Tennessee. I obviously could not run, but it was possible to walk 13.1 miles in the four-hour time limit, so I was going to try. It was one of the most difficult things I have done, but I crossed the finish line just under the wire.
9. What problems or disabilities, if any, resulted from your brain injury
(e.g., balance, perception, personality, etc.)?
Looking at computer and phone screens for extended periods of time increases my migraines. I still have to rest more than healthy people, and my vision will get blurry if I do not rest in time. Socializing exhausts me, and I often spend the next day in bed with a migraine. Since my hypothalamus was compromised during surgery, I experience frequent hot and cold flashes. (The hypothalamus helps regulate the body’s core temperature.) I get overheated and feel like I cannot breathe, but when I take just my socks or sweatshirt off, I can start shivering and feel chilled to the bone within a minute or two. I used to love the heat of summer, but now it makes me sick if I spend much time in it.
10. How has your life changed? Is it better? Is it worse?
My life is immensely better than it was the few years before my surgery. At that point, I wasn’t really living; I was simply existing. I have been able to offer advice and encouragement to others who were going to undergo brain surgery. Without my experiences, I would not have had those opportunities. I also recently published a book called 30 Days to Understanding Chronic Illness and Pain.
11. What do you miss the most from your pre-brain-injury life?
Besides just feeling healthy, I used to be active and fit. Working out gave me an energy boost and made me feel better, like it is supposed to. Now, I still try to exercise and I love hiking, but those things exhaust me. I often have to nap right afterward, and physical exertion can make my head hurt and feel foggy.
12. What do you enjoy most in your post-brain-injury life?
Besides my brain injury, I have other chronic illnesses. I believe that if I want people to understand, then it is my job to teach them (with patience and kindness). Of course, not everyone is willing to listen; but if I do not at least try, then I am not even giving them the opportunity. Navigating through the limitations and suffering can be discouraging. In addition to the symptoms themselves, the stigmas and misconceptions may seem insurmountable. My goal for my book is for it to be an easy and informal read that covers a wide range of topics, including invisible illnesses, cost, guilt and loneliness, fatigue, brain fog, pacing, prevalence, and more. My hope is that it will help me help healthy people gain a better understanding of what life with chronic illness and pain is really like, while also offering support and encouragement to those who are struggling.
13. What do you like least about your brain injury?
See above.
14. Has anything helped you to accept your brain injury?
No answer
15. Has your injury affected your home life and relationships and, if so, how?
No answer
16. Has your social life been altered or changed and, if so, how?
See above.
17. Who is your main caregiver? Do you understand what it takes to be a caregiver?
No answer
18. What are your plans? What do you expect/hope to be doing ten years from now?
See above.
19. Are you able to provide a helpful hint that may have taken you a long time to learn, but which you wished you had known earlier? If so, please state what it is to potentially help other survivors with your specific kind of brain injury.

I wish I would not have stayed silent about my struggles for so long. I used to avoid talking about my pain and the journey that I was on. I do not like to complain, and I know that everyone has challenges in life. But as I slowly began to open up, people came out of the shadows. I realized that I was not alone in feeling alone and that others were going through the same or similar things. When we keep our suffering to ourselves, it can steal our entire focus and limit outside interests and distractions. This can lead to feelings of hopelessness, resentment, or loneliness. There is no shame in seeking therapy or other support to help you develop coping skills. While you may not be able to control the pain or limitations themselves, you can take control of how you deal with them.
20. What advice would you offer to other brain-injury survivors? Do you have any other comments that you would like to add?
Rest is not laziness, and pacing is vital. We live in such a fast-paced world, and there is always so much to do. One of the hardest lessons to learn is to slow down because you cannot do everything that you used to. It is easy to feel guilty, lazy, or left out. It is difficult to leave projects unfinished and to stay home when everyone else is out having fun. But once your body informs you that you are overdoing it, you need to rest and stop comparing yourself to others. When you rest because your body is weak, you are not wasting time doing nothing. You are doing exactly what you need to do. You are recovering.
Get Your Copy Now!
Read It! Listen to It! Review It!
Click Links under Book
PAPERBACK! Read it Now!
e-BOOK! Read it Now!
AUDIO BOOK Listen to it Now!
Stay Safe and Healthy!
Clip Art compliments of Bing.)
(Photos compliments of contributor.)
As I say after each post:
Please leave a comment by clicking the blue words “Leave a Comment” below this post.
Feel free to follow my blog. Click on “Follow” on the upper right sidebar.
If you like my blog, share it intact with your friends. It’s easy! Click the “Share” buttons below.













 10. How has your life changed? Is it better? Is it worse?
10. How has your life changed? Is it better? Is it worse?
 e. ACCEPT THAT LIFE ISN’T FAIR. We need emotions to help us learn. Grow towards the light. Don’t become a weed and strangle those next to you. Treat others as you would want to be treated.
e. ACCEPT THAT LIFE ISN’T FAIR. We need emotions to help us learn. Grow towards the light. Don’t become a weed and strangle those next to you. Treat others as you would want to be treated.





 18. What are your plans? What do you expect/hope to be doing ten years from now?
18. What are your plans? What do you expect/hope to be doing ten years from now?















 What is your name? (last name optional)
What is your name? (last name optional)

 When Jordan first came home from rehab, she required help with most of her ADLs (Activities of Daily Living). As time has gone on, she has been able to perform most of her ADLs on her own. She has short-term memory loss, so my role is helping to make sure that she remembers things and stays safe.
When Jordan first came home from rehab, she required help with most of her ADLs (Activities of Daily Living). As time has gone on, she has been able to perform most of her ADLs on her own. She has short-term memory loss, so my role is helping to make sure that she remembers things and stays safe.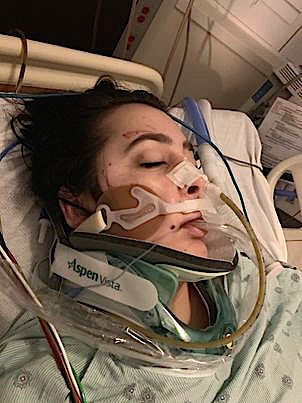


 18. What are your plans? What do you expect/hope to be doing ten years from now?
18. What are your plans? What do you expect/hope to be doing ten years from now? 20. What advice would you offer to other brain-injury survivors? Do you have any other comments that you would like to add?
20. What advice would you offer to other brain-injury survivors? Do you have any other comments that you would like to add?






 Even though we’ve been vaccinated, we are still being careful. We try to mix with vaccinated people only. We try to avoid people and places that might be hot spots for infection. We only eat on restaurant patios; we never eat inside. We still practice social-distancing when we can, and we still wash our hands thoroughly and use disinfectant if we can’t wash our hands.
Even though we’ve been vaccinated, we are still being careful. We try to mix with vaccinated people only. We try to avoid people and places that might be hot spots for infection. We only eat on restaurant patios; we never eat inside. We still practice social-distancing when we can, and we still wash our hands thoroughly and use disinfectant if we can’t wash our hands.


Recent Comments